OVERVIEW
During a total hip replacement (THR), the arthritic or damaged joint is removed and replaced with an artificial joint that moves just like a healthy hip. Both the head of the femur (ball on-top of the thigh bone) and the acetabulum (hip socket) are both replaced. A metal stem (often titanium) is implanted into the femur and femoral head is replaced with an artificial ceramic ball, which attaches to the metal stem. The hip socket (into which the ball fits) is replaced with a titanium shell with an artificial liner made of ceramic or hardwearing polyethylene (which sometimes can be fixed directly with bone cement). These surfaces that move together are known as the ‘bearing’ and allow for smooth and painless movement of the ball in the socket.
The artificial joint may be cemented in position or press-fitted securely in place without cement (uncemented). The length of stem used in Total Hip Replacement can also vary from traditional, longer stems to shorter contemporary, bone conserving stems.
What type of replacement is right for you? Different options for hip replacement are available and can be summarised as follows:
- Short Stem Total Hip Replacement
- Uncemented Total Hip Replacement
- Cemented Stem (Hybrid) Total Hip Replacement
- Fully Cemented Total Hip Replacement
Short Stem
A short stem hip replacement uses a shorter femoral implant (in comparison to the longer stems used in traditional THR). The acetabulum (socket) is replaced as normal with a bearing suitable to the patient.
Mr Stafford often uses MiniHip™ and Trifit™, which are both clinically proven, bone-conserving implants. Its shape provides a natural fit inside the femur and a better distribution of the load compared with some conventional femoral stems. This improves revision options for patients who may need further treatment in later life.
Uncemented
‘Cementless’ or ‘uncemented’ stems do not require bone cement in order to fix them in place – the surface of the implant is instead covered in a special (hydroxyapatite) porous coating which helps to fix the prosthesis securely in position. Over a few weeks, the patient’s natural bone grows through the pores, attaching the artificial joint to the hip’s natural remaining bone structure. Cementless hydroxyapatite coatings are used on both short stems and longer, traditional stems.
Cemented
Cemented total hip replacements are considered gold standard in many countries. The stem is fixed in position inside using bone cement, which holds it securely in position inside the femur. These types of hip replacement have been shown to last many years.
Hybrid hip replacements combine the use of a cemented femoral stem with an uncemented acetabular cup. The benefit of this is that it allows the use of more contemporary bearings such as ceramics.
An artificial acetabular ‘cup’ or ‘shell’ sits inside the hip socket, and provides a new surface for this section of the hip joint. The ball at the head of the femoral stem fits inside this shell.
Mr Stafford prefers Corin’s Trinity™ acetabular system. This consists of a titanium hemispherical shell with an inner polyethylene or ceramic liner. It is an ‘uncemented’ design utilising the hydroxyapatite coating mentioned above. Over time, the natural bone grows through the pores, attaching to the hip’s remaining bone structure. The inner polyethylene or ceramic lining articulates against the ball at the head of the femur, allowing for smooth movement of the artificial joint.
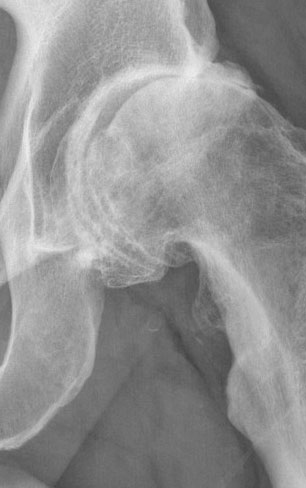
Hip Arthritis
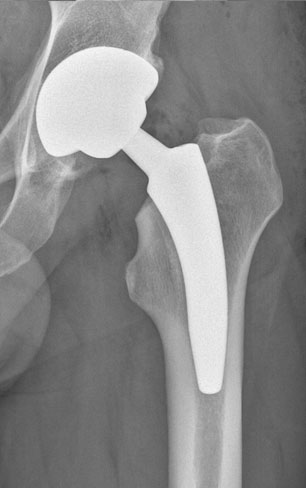
MiniHip
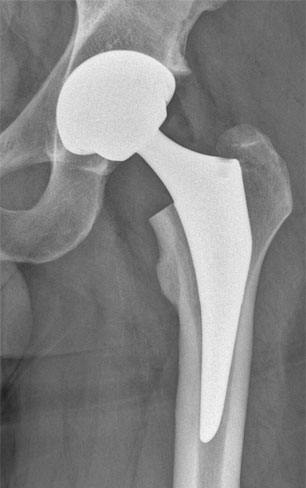
Trifit
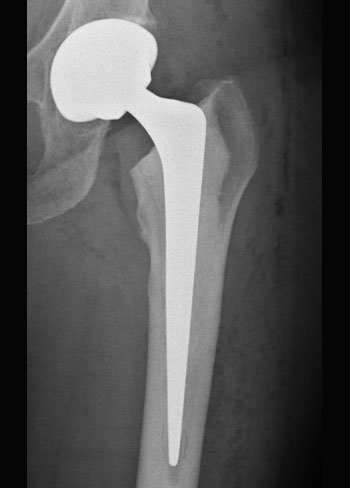
Hybrid Hip
Replacement
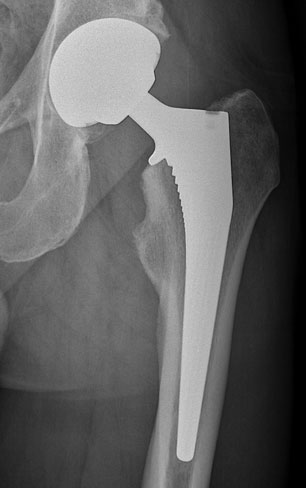
Uncemented Hip Replacement
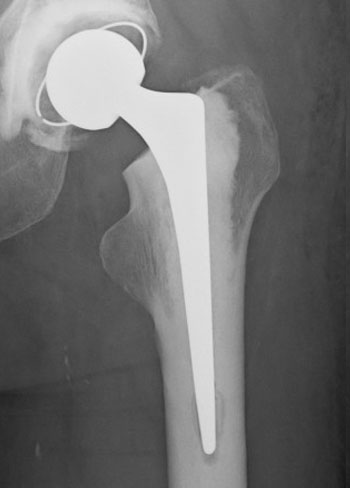
Cemented Hip
Replacement
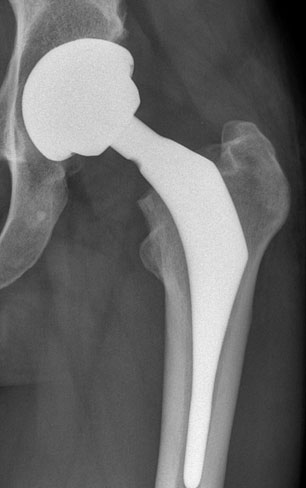
Custom Hip
Designs (including Resurfacing)
The phrase ‘Total Hip Replacement’ (THR) refers to an operation performed for hip arthritis (joint wear and tear). In general terms, the procedure involves placing a new prosthetic cup into the acetabulum (the cup or socket of the hip joint) and replacing the femoral head (ball of the hip) with a new one. There are many different designs available, ranging from resurfacing to revision-type components.
All THR designs are secured to the patients’ host bone by either cemented or uncemented means. Cemented hip replacements were popularised by Charnley in the 1960’s and became the ‘gold standard’ over the years. The problem with cemented components is that over time the cement may become damaged by repetitive loading, or work its way loose from the surrounding bone. However, this is only really an issue in very active ‘high-demand’ patients, who want to continue with sports or other physically demanding activities. The problem is that more and more people are wearing out their joints at a younger age due to increasingly active lifestyles and sporting endeavours.
Therefore, surgeons have always searched for a hip that may better withstand the rigours of active life, for those who wish to continue to play tennis etc. One possible solution is if you can get the implant to be better bonded to the host bone. For this reason, uncemented Hip Replacements have become increasingly popular in younger, more active patients. Most have a special coating, which the bone can grow onto so that it becomes a part of the patient, and can therefore theoretically withstand much higher forces.
Most of the uncemented designs are, however, reasonably new to the market in relation to their cemented counterparts and so we cannot necessarily state the 15 or 20-year survivorship. A small number of uncemented stems have been available for this period, such as the JRI Furlong and the DePuy Corail; the survivorship of these stems are among the best of all femoral components. The problem with these types of designs just mentioned is that they are not particularly bone conserving. To place them into the native femur, the surgeon has to remove quite a lot of the central bone, possibly broaching up to 15cm (6 inches) into the femoral canal. Although this in itself is not an issue, if the patient does wear it out and it becomes loose, then often an even larger component has to be implanted to gain implant stability.
As a result of this, surgeons who have a younger patient population have looked towards more bone conserving designs, to keep options in the event of the hip replacement wearing out. The most famous of these is the Birmingham Hip Resurfacing (currently manufactured by Smith & Nephew). The idea behind this was that if it does wear out, or there is a problem with it, it could easily be converted to a standard primary type of Total Hip Replacement, rather than a larger revision-type component. This may gain the patient an ‘implant generation’.
Although the BHR (and other resurfacing designs) is bone conserving on the femoral side, quite often the surgeon needs to remove more of the acetabular (pelvic) bone than normal to accommodate the large socket needed with the larger heads used. This can be a problem when it comes to revising them. Also, the range of motion following resurfacing is commonly not what one would like, due to the decreased offset between the hemispherical cup and femoral neck. There are other issues as well, such as persistent psoas irritation (a muscle that runs over the front of the hip). All resurfacing designs utilise a metal-on-metal bearing, which can be a problem and discussed in ‘Bearings’.
As resurfacing has become less popular, other designs of bone conserving stems and cups have now been made available in the UK, some which have been around for some time before UK release. The benefits of most of these designs are that they may be both bone conserving on both the socket and the femur. This also gives the advantage of a better range of motion, uncemented technology, bone conservation and utilisation of ceramic on ceramic components (see Bearings).
BEARINGS
 In conventional Total Hip Replacement designs, a metal ball articulates with a plastic (polyethylene) cup. The plastic cup is not usually hard enough to cause metal ball wear, but the ball does wear the plastic cup away. Thus, in general terms, a plastic bearing will always wear out at some stage, albeit in a predictable and slow manner. Not only do standard plastic cups eventually fail, the particles of plastic, which are released from the frictional wear, can cause local bone resorption (osteolysis). This loss of bone can often be an issue when revising these types of Total Hip Replacement, and often bone graft (substitute bone) needs to be used to fill the defects. One strategy to slow the wear of the plastic cup is to substitute the metal ball for a smoother ceramic ball, which causes less frictional wear and may prolong the life of the plastic liner. Also, newer harder ‘cross-linked’ plastics have become available which also look to slow the wear rate. We now have data to show the wear rates of the newer cross-linked poly liners is very low, and as a result we can expect ceramic-on-cross-linked poly hip replacements to last 20 years or more.
In conventional Total Hip Replacement designs, a metal ball articulates with a plastic (polyethylene) cup. The plastic cup is not usually hard enough to cause metal ball wear, but the ball does wear the plastic cup away. Thus, in general terms, a plastic bearing will always wear out at some stage, albeit in a predictable and slow manner. Not only do standard plastic cups eventually fail, the particles of plastic, which are released from the frictional wear, can cause local bone resorption (osteolysis). This loss of bone can often be an issue when revising these types of Total Hip Replacement, and often bone graft (substitute bone) needs to be used to fill the defects. One strategy to slow the wear of the plastic cup is to substitute the metal ball for a smoother ceramic ball, which causes less frictional wear and may prolong the life of the plastic liner. Also, newer harder ‘cross-linked’ plastics have become available which also look to slow the wear rate. We now have data to show the wear rates of the newer cross-linked poly liners is very low, and as a result we can expect ceramic-on-cross-linked poly hip replacements to last 20 years or more.
Hip resurfacing, and other metal-on-metal (MoM) designs, have recently been subject to much media speculation regarding ‘metal allergy’. Other phrases which have also been used are ALVAL, and most recently ARMD (Adverse Reaction to Metal Debris). As one walks on any type of THR, there will be a small amount of particulate debris released from wear between the ball and cup (or cup liner) as the ball rubs against the cup. In some patients, the metal released into the hip joint (usually cobalt and chrome) can cause a local allergic reaction. This can cause damage to the muscles surrounding the hip, and if very advanced, even the bone. This damage is irreversible, and can also be silent (the patient is not aware of a problem), until quite advanced destruction has occurred. At this point, the results of revision of the components is always disappointing, as although the surgeon can eradicate the metal reaction by removing the components and affected tissue, they may not reconstitute the lost muscle. As a result, I do not perform any form of metal-on-metal hip replacements.
My ideal strategy to prolong the life of the Total Hip Replacement is to use a ceramic ball on a ceramic liner (ceramic on ceramic, or CoC). There are many advantages to this coupling. The wear debris does not cause any local reaction in bone or muscle. The wear rates are extremely low and it has an excellent chance of lasting a young patient’s lifetime. The surgeon can use larger heads, which impart greater stability (one of the perceived advantages of MoM). The downsides are that the components are very expensive, and historically there has been reported incidences of the ceramic squeaking or even breaking.
Ceramic components have been used for around twenty years now, however. They have evolved (we are now on the fourth generation, released in 2003) so that they are now much less brittle (difficult to break or shatter) and therefore can withstand much higher impact forces. The incidence of squeaking is extremely low, and does not necessarily mean that there is a problem with the components. However, there was a particular type of CoC THR that was widely used, especially in the USA, which had a very high rate of squeaking. This was due to a design issue of those particular components, but as a result, all CoC components gained a bad name for this. Thankfully, in Europe and the rest of the world, this has not been seen in any significant numbers and so we have continued to be able to use them with great success.
As a result of all of the above, my personal strategy for successfully treating the active patient for whom joint preservation keyhole surgery is not suitable, a bone conserving design coupled with a CoC bearing is the implant of choice. However, all patients are treated on a case-by-case basis, and not everyone is suitable. Rest assured, however, that whatever we decide upon (between the patient and surgeon) will be the best option for you.
Optimised Positioning System (OPS)
Laser guided, personalised solutions for hip replacement surgery
This is an innovation designed to improve the long-term outcome of hip replacements. The rationale is to determine what exact angles the acetabular shell should be placed in the pelvis, determined by your own anatomy and the way you move. It requires three extra x-rays and a CT scan over the normal imaging that is required for pre-operative planning. A personalised instrument is manufactured (3D printed) which fits inside your pelvis and uses a laser to indicate where Mr Stafford and the analysts and have agreed is best for you.
Mr Stafford may offer this to you if he feels that your case is suitable. However, it takes about four weeks to manufacture and also exposes the patient to more radiation (from the x-rays and scan) than normal. However, early research has demonstrated that this system may reduce the risks of squeaking and dislocation following surgery.
TOTAL HIP REPLACEMENT FAQs
This is a difficult question as obviously it depends on the nature and length of the flight. Short haul flights should be okay after approximately 6 weeks, and long haul flights after around 3 months. However, we can discuss this is more detail in person if needed.
You should see a physiotherapist within the first week or two following your operation.
In a perfect world people take around 6 weeks off work but a lot of people are unable to do this. If your work is flexible I would suggest 6 weeks is just right, however I have a large cohort of people who have gone back to work after just a week or two. This is not, however, my advice.
You should leave your dressings in situ until you are seen in clinic by Mr Stafford who will take your dressings off himself.
There is in fact no law about this. It depends on which leg has been operated on as the main issue is your reaction time should you need to perform an emergency stop. You should always check with your insurance company as some have stipulations but the advice from a medical perspective is that you can drive when you yourself feel safe to do and that you can perform an emergency stop in a timely manner as you would have done pre-operatively. Around 6 weeks.
I routinely do not prescribe crutches for a specific length of time. Also, different physiotherapists will give different advice about this. My personal feeling is that you should use them for as long as you personally feel that you need them, and I am happy for you to discard your crutches whenever you feel you are safe to do so. This is normally somewhere between 2 and 4 weeks post-operatively but obviously there is variation between patients.
I personally feel that you should leave any form of sports of significant physical exercise for approximately 3 months to allow the implant to be fully integrated and to allow the soft tissues to recover. Obviously this depends on the sport and we can discuss this in person if needed.
For more answers to your questions, click on the link below!

Your Total Hip Replacement –
A Surgeon’s guide for patients
Please download this free guide for patients to hip surgery
Please be aware that the information contained in the guide is a general in nature and should not be considered medical advice.
RECOGNISED BY ALL THE MAJOR INSURERS


